Hello. I am Dr. Dongkyu Lee, an orthopedic specialist. Patients often ask whether they absolutely need an MRI for shoulder conditions. What do you think? I have previously written about this topic and will share the links below. https://blog.naver.com/9690067/221514139192
🔗 https://blog.naver.com/9690067/221514139192https://blog.naver.com/9690067/221417655749
🔗 https://blog.naver.com/9690067/221417655749In conclusion, ultrasound alone is sufficient for diagnosing rotator cuff conditions. When examining a patient, I first listen carefully to their symptoms and perform a physical examination. The physical examination can provide a reasonable estimate of which tendon is affected, and whether the problem is inside or outside the joint. If the physical examination suggests only a rotator cuff problem, ultrasound alone is sufficient for diagnosis. Of course, if the physical examination suggests an intra-articular problem or labral issue, MRI is necessary. Since ultrasound cannot penetrate solid structures, it cannot visualize the interior of the joint. However, the rotator cuff consists of tendons sitting on top of bone, so ultrasound can diagnose them more precisely. MRI typically captures images in 4mm slices, making it difficult to diagnose lesions smaller than 4mm or fine calcifications. Ultrasound provides real-time video and allows continuous observation of the tendons. Let's compare the two.
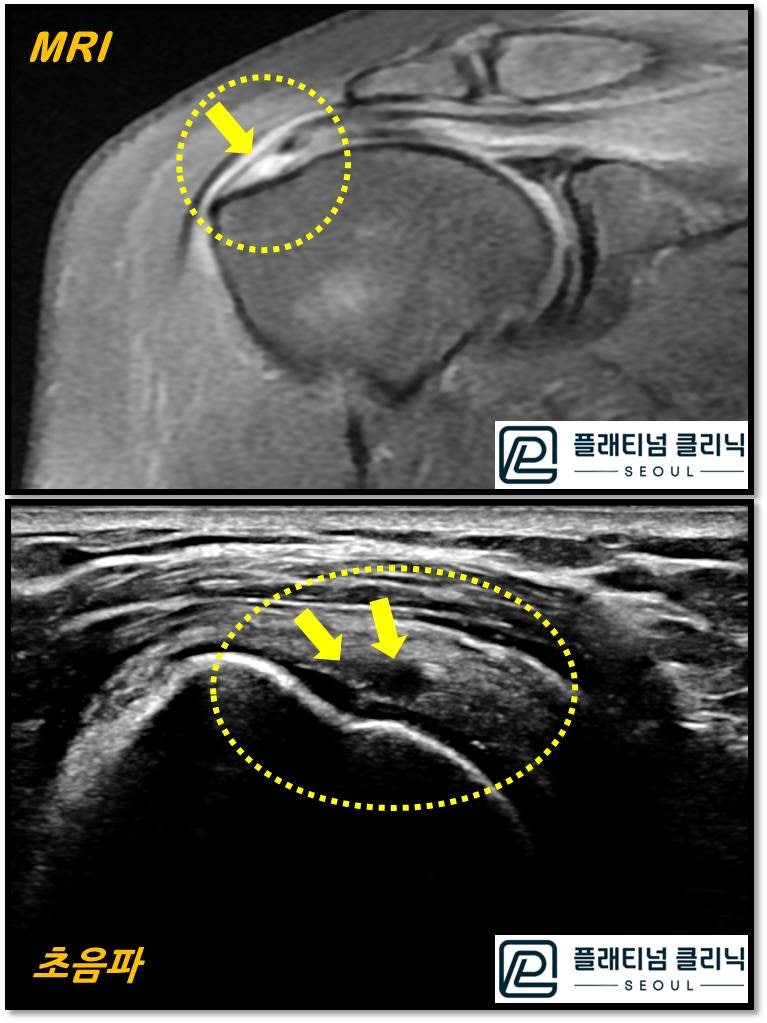
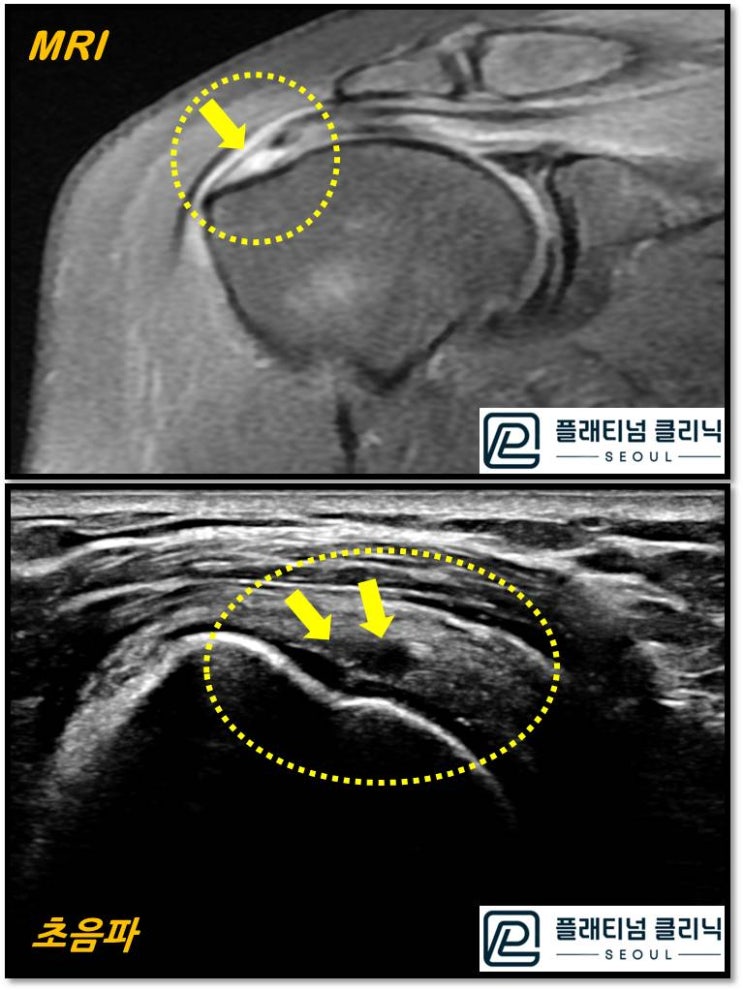
This image compares MRI and ultrasound for a rotator cuff tear. The upper image is MRI and the lower is ultrasound. The torn area is indicated by the arrow within the yellow circle. On MRI, the tendon appears dark and the tear appears white. On ultrasound, the tendon appears white and the tear appears dark. Which looks better to you? To me, the ultrasound appears clearer and larger. The tendon substance is well visualized, and the muscle fiber direction is clearly observed. Of course, having performed ultrasound for many years, my proficiency may contribute to finding it easier to read.
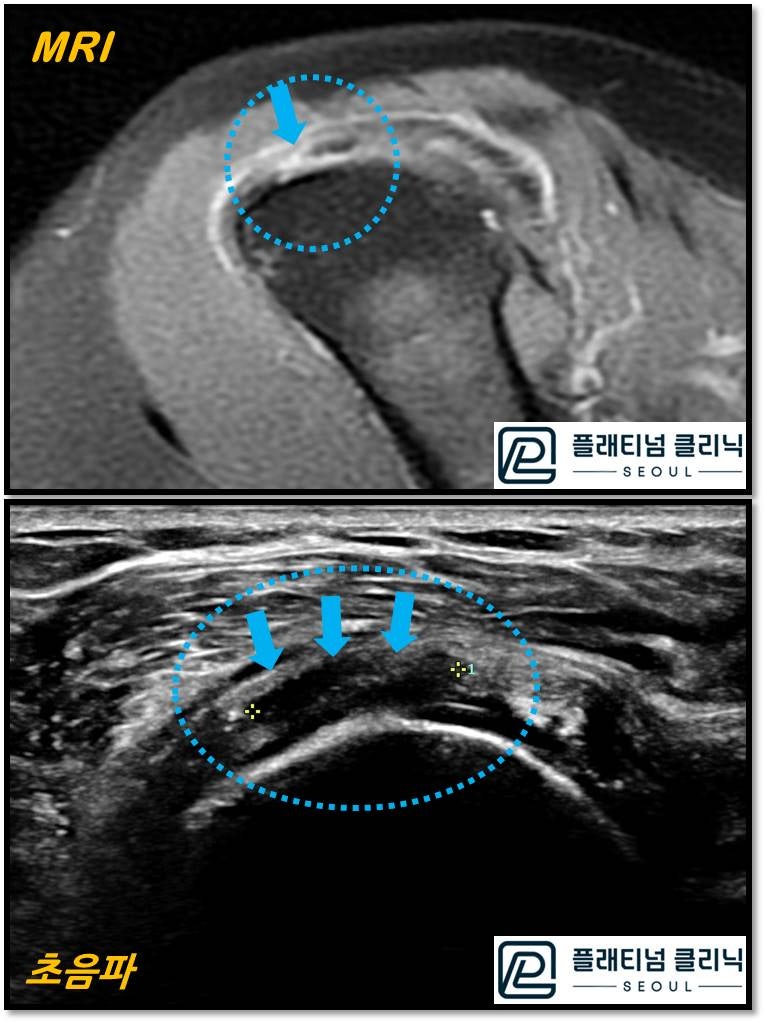
This is a cross-sectional comparison of the same patient's rotator cuff tear. At a glance, doesn't the ultrasound appear larger and clearer? The torn area is much more clearly visible. Beyond this, because ultrasound provides continuous examination, it can diagnose fine calcifications, inflammation, and tears better than MRI. MRI is better at diagnosing large tears or large calcifications (4mm or more), but struggles with smaller lesions. Of course, results can vary depending on the ultrasound operator. An experienced orthopedic surgeon can sufficiently diagnose rotator cuff conditions with ultrasound alone, without MRI.
In conclusion, ultrasound alone is sufficient for diagnosing rotator cuff conditions.