A 65-year-old male patient presented with knee pain that had persisted for several years. Despite years of cartilage injections, medication, and physical therapy, no treatment provided improvement, leading him to visit Platinum Clinic. Physical examination revealed positive Apley external rotation and tenderness along the medial joint line.
X-ray showed narrowing of the medial joint space with signs of arthritis.
Based on the physical examination findings suggesting medial meniscus damage, an MRI was performed to assess the exact condition of the joint.
Degenerative tear of the medial meniscus from the mid-body to the posterior horn was observed, along with loss of the medial femoral cartilage.
The patient was found to have a medial meniscus tear, medial femoral cartilage damage (arthritic change grade IV), and mild varus deformity. While the patient's age of 65 is somewhat elderly, the condition was otherwise nearly normal. Therefore, the decision was made to perform a proximal tibial osteotomy (axis correction), chondroplasty, and partial meniscectomy.
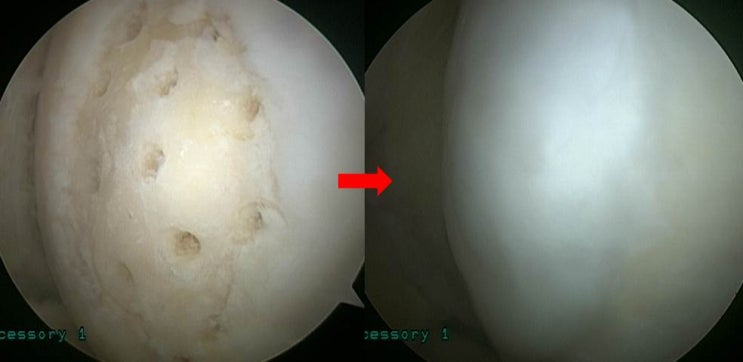
Arthroscopy revealed abnormal findings of the medial femoral cartilage, which was debrided and treated with chondroplasty. A complex degenerative tear of the medial meniscus was observed, and a partial meniscectomy was performed to smooth the meniscal surface.
Proximal tibial osteotomy was performed.
Post-operative imaging confirmed that the mechanical axis was accurately corrected from the medial side to a slightly lateral position.
One year later, hardware removal and arthroscopy were performed.
As seen in the right image, the cartilage has regenerated perfectly, as if new tissue has grown in.
Even in elderly patients, if the axis is accurately corrected and appropriate chondroplasty is performed, excellent results like this can be achieved. I recall the patient visiting a few days ago -- he had had a few drinks (please do not drink alcohol during treatment!) and came by to express his gratitude, which truly made my day.